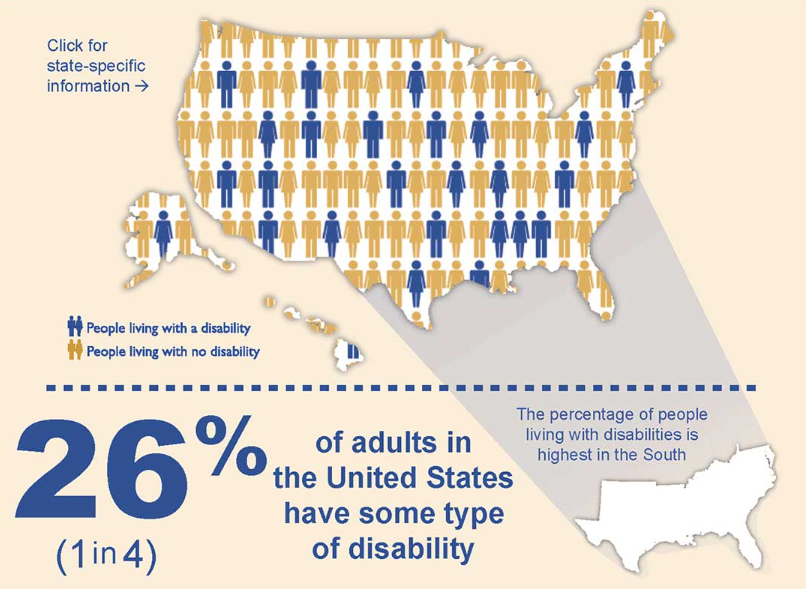
Healthcare for people with disabilities in the United States is a complex and evolving issue that intersects with social justice, public policy, economics, and human rights. Individuals with disabilities represent a significant portion of the U.S. population, with estimates suggesting that over 60 million Americans live with some form of disability. These disabilities may be physical, sensory, intellectual, developmental, or psychological in nature. Ensuring equitable access to healthcare for this population is not only a moral obligation but also a critical component of building an inclusive and healthy society. Despite progress in legislation and awareness, substantial barriers remain, affecting the quality, accessibility, and affordability of healthcare for people with disabilities.

One of the foundational aspects of healthcare for people with disabilities in the United States is the legal framework designed to protect their rights. The Americans with Disabilities Act (ADA) of 1990 is perhaps the most significant piece of legislation in this regard. It prohibits discrimination against individuals with disabilities in various areas, including healthcare services. The ADA mandates that healthcare providers offer reasonable accommodations to ensure equal access. This includes accessible facilities, communication aids such as sign language interpreters, and modifications in procedures when necessary. Additionally, Section 504 of the Rehabilitation Act of 1973 and the Affordable Care Act (ACA) further reinforce these protections by expanding access to insurance coverage and prohibiting discriminatory practices in healthcare settings.
Despite these legal protections, people with disabilities often face systemic barriers when accessing healthcare services. One of the most prominent challenges is physical accessibility. Many healthcare facilities, especially older ones, are not fully equipped to accommodate individuals with mobility impairments. Examination tables, diagnostic equipment, and even entrances may not meet accessibility standards. This can result in delayed or inadequate care, as patients may avoid seeking medical attention due to these obstacles.
Another major barrier is communication. Individuals with hearing, vision, or cognitive impairments may struggle to communicate effectively with healthcare providers. While the ADA requires accommodations such as interpreters or accessible formats, these services are not always consistently provided. This gap can lead to misunderstandings, misdiagnoses, and reduced quality of care. For example, a deaf patient who does not have access to a qualified interpreter may not fully understand their diagnosis or treatment plan, which can have serious health consequences.
Financial challenges also play a significant role in limiting access to healthcare for people with disabilities. Many individuals with disabilities rely on public insurance programs such as Medicaid and Medicare. While these programs provide essential coverage, they often have limitations in terms of provider availability, covered services, and reimbursement rates. Additionally, individuals who are not eligible for these programs may struggle to afford private insurance due to high premiums and out-of-pocket costs. The ACA has helped expand coverage, particularly through Medicaid expansion in many states, but gaps still remain, especially in states that have not adopted expansion policies.
Another critical issue is the shortage of healthcare providers who are adequately trained to care for patients with disabilities. Medical education in the United States has historically placed limited emphasis on disability-specific care. As a result, many healthcare professionals may lack the knowledge and confidence needed to provide appropriate treatment. This can lead to biases, both conscious and unconscious, that affect clinical decision-making. Some providers may incorrectly assume that a patient’s disability is the primary cause of their symptoms, overlooking other potential health conditions. This phenomenon, known as “diagnostic overshadowing,” can result in delayed or incorrect diagnoses.
Mental health is another area of concern. People with disabilities are more likely to experience mental health challenges such as depression and anxiety, often due to social isolation, stigma, and barriers to participation in daily activities. However, access to mental health services can be particularly difficult. There is a shortage of mental health professionals, and even fewer are trained to work with individuals with disabilities. Furthermore, insurance coverage for mental health services may be limited, and accessibility issues can further complicate access to care.
Technology has the potential to significantly improve healthcare access for people with disabilities. Telehealth, for instance, has emerged as a valuable tool, particularly during the COVID-19 pandemic. Virtual consultations can reduce the need for transportation and make it easier for individuals with mobility challenges to receive care. Assistive technologies, such as speech-to-text software, screen readers, and remote monitoring devices, can also enhance communication and independence. However, the digital divide remains a concern, as not all individuals have access to reliable internet or the necessary devices.
Transportation is another critical factor affecting healthcare access. Many people with disabilities face challenges in traveling to medical appointments due to a lack of accessible transportation options. While some communities offer paratransit services, these are often limited in availability and flexibility. Missed appointments due to transportation issues can lead to worsening health conditions and increased healthcare costs in the long term.

Cultural and social factors also influence healthcare outcomes for people with disabilities. Stigma and discrimination can discourage individuals from seeking care or advocating for their needs. In some cases, healthcare providers may unintentionally perpetuate these biases, leading to unequal treatment. Addressing these issues requires not only policy changes but also a shift in societal attitudes toward disability. Promoting disability awareness and inclusion can help create a more supportive healthcare environment.
The role of caregivers is another important aspect of healthcare for people with disabilities. Many individuals rely on family members or professional caregivers for assistance with daily activities and medical needs. Caregivers play a crucial role in coordinating care, managing medications, and providing emotional support. However, they often face significant challenges, including financial strain, burnout, and a lack of support services. Strengthening support systems for caregivers is essential to improving overall healthcare outcomes.
Policy reforms and advocacy efforts continue to play a vital role in addressing these challenges. Disability rights organizations have been instrumental in pushing for changes in legislation, funding, and public awareness. Initiatives aimed at improving accessibility, expanding insurance coverage, and enhancing provider training are essential steps toward a more equitable healthcare system. For example, some states have implemented programs to incentivize healthcare providers to receive training in disability care. Others have expanded home- and community-based services, allowing individuals to receive care in more comfortable and familiar environments.
Preventive care is another area that requires attention. People with disabilities are less likely to receive routine screenings and preventive services, such as cancer screenings and vaccinations. This disparity can lead to higher rates of chronic conditions and more severe health outcomes. Efforts to improve preventive care must address both accessibility and awareness, ensuring that individuals with disabilities receive the same level of preventive services as the general population.
In recent years, there has been a growing recognition of the importance of person-centered care. This approach emphasizes the preferences, needs, and values of the individual, rather than focusing solely on their disability. By involving patients in decision-making and tailoring care to their unique circumstances, healthcare providers can improve both satisfaction and outcomes. Person-centered care also aligns with the broader goal of promoting independence and quality of life for people with disabilities.
Research and data collection are also critical for improving healthcare for people with disabilities. Accurate and comprehensive data can help identify disparities, inform policy decisions, and evaluate the effectiveness of interventions. However, people with disabilities have historically been underrepresented in medical research, leading to gaps in knowledge. Increasing their inclusion in clinical trials and health studies is essential for developing evidence-based practices that meet their needs.
In conclusion, healthcare for people with disabilities in the United States is a multifaceted issue that requires coordinated efforts across multiple sectors. While significant progress has been made through legislation and advocacy, many challenges remain. Addressing these challenges will require continued investment in accessibility, education, technology, and policy reform. It will also require a commitment to equity and inclusion, ensuring that all individuals, regardless of their abilities, have access to high-quality healthcare. By prioritizing these efforts, the United States can move closer to a healthcare system that truly serves everyone.
Get New Articles Every Week
Subscribe to receive the latest WordPress and SEO tips.